Tale of a Tonsillectomy
Whitney had her tonsils out. Poor sweet girl didn’t know what was coming…and neither did we.
Originally, we had a surgery scheduled just to put ear tubes in – an outpatient procedure, she’s done it before, involves anesthesia which nobody likes, but other than that a pretty simple deal. She was getting tubes put in (again) because for the past 6 months she has consistently had fluid in her ears – and fluid in the ear muffles sound, she had low scores on hearing tests and while it was difficult to detect any trouble hearing in her behavior (she works really hard to pick up other cues to keep up with what’s going on), not being able to hear is a serious detriment to learning, and particularly speech development. Duh. She needs to be able to hear. She’s 4.5 yrs old, often by this age kids “age out” of ear tubes as their ear canals have developed to drain more efficiently. We were hoping that would be the case, but not so with our girl (and often not so with kids with Down syndrome). Bring on the tubes.
Because it was her second time getting tubes her (new and fabulous) ENT suggested we consider other reasons she might have chronic fluid – particularly, that drainage between her ears, nose and throat might have blockages due to enlarged adenoids. We planned to have the ENT take a look at her adenoids (in the back of the nasal passage) and “melt them away” or so she described, if indeed they were large enough to be contributing to a blockage. Adenoids apparently don’t serve much of a purpose in and of themselves, there is supposedly no drawback to being adenoid-free. Sure, melt them, we said.
Finally, since Whitney was going to be under anesthesia already, the ENT suggested we get a sleep study. She saw in the notes that about a year ago we asked our former ENT about one – thinking that maybe she was breathing irregularly during sleep – but then we didn’t follow through with it. At the time, I kept listening to her when I lay down with her and thought that she doesn’t really snore, and maybe the breathing had to do with being sick…perhaps her breathing wasn’t really that irregular. She wasn’t gasping for air or waking up choking or anything, so I doubted she had apnea or anything. Boy was I wrong. We went through with the sleep study – a rush order per her ENT’s request. I’ll have to write more about it in another post because the whole experience was rather interesting. What they found was that she had severe sleep apnea – the results were so bad that there was no question we needed to get her tonsils out of there and so the morning of the surgery it was decided that she’d get the ENT trifecta (tubes, adenoidectomy, tonsillectomy). The kicker was that we really weren’t prepared for the tonsil part – we hadn’t researched the surgery or recovery, knew it was a much bigger deal but hadn’t planned for all the pain management nor adjusted our schedule for laying low for the rest of the week. The hope was to take care of all that needed fixing with one session of anesthesia – we certainly didn’t want to come back and do all the fasting and hospital scene another time if we could take care of everything at once.
Pre-op with Mommy / Post-op with Daddy 
The surgery went fine (minus more than half a dozen bruises and sore spots all on her arms/legs/hands/feet from where they clearly were looking for a vein and couldn’t find one). Tyler played super daddy with Whitney almost the whole time (receiving the anesthesia, being there when she woke up, and ultimately spending the night with her there in the hospital for recovery). I hung in the waiting rooms and hospital cafeteria entertaining Dylan and got to trade off to see my little girl in recovery. She was clearly pretty miserable. Whimpering, trying to talk but in a lot of pain. I can only imagine how scared it must be to wake up and know something major has happened to you but not really understand what (or to have the understanding and hope that it will get better with time!). We had tried to talk with her about how she was going to have the doctors help her be able to breathe, hear, and sleep better, and that her throat will be a bit ouchy for a while but that it will get better, but I’m sure that did little to prepare her for the actual experience. It feels so cruel and heartbreaking as a parent to hand off your sweet baby to someone to do something that will hurt them – even when you know that the pain is necessary in the short term for a longer term benefit. This was Whitney’s third time in surgery and I truly hope it is her last. I’d like to think that we’ve all earned our *surgery/hospital* badge by now.
Whitney did really well the first few days of recovery. She was drinking and eating immediately after surgery. She took her oral pain killers like a champ (just Tylenol and Motrin around the clock). She would try to talk – and still had a little bit of play in her.
Watching movies and enjoying popsicles after being moved to a room for the night.
The next few days at home started off nicely – we would wake her up in the middle of the night for doses of meds to keep ahead of the pain, she had reasonable energy for playing and dancing. Dylan got a fever and cough almost immediately after the surgery…as much as I tried to hand sanitize every 10 minutes he was all over the place, so I wasn’t all that surprised. I soon also got a cough (no fever) and within a few days Whitney had a little cough too (but nothing like Dylan’s, and fever was nothing like Dylan’s either). She was running a little warm but that was to be expected post-surgery. I also wondered if maybe the cough could be related to drainage from spit/surgery site.
Pretty soon we had to fight Whitney to get her medicine down – she started to squirm away from the syringe or would let the medicine pool up in her mouth and would spit it out. Without full doses of medicine it was also clear she was in more and more pain. One night I even tried to plug her nose to get her to swallow the medicine – desperate for her to get back on the cycle of having her pain managed. She fought it so hard she made herself throw up. It was terrible. Quickly, things got pretty bad. She was refusing to eat or drink anything…we kept checking for wet diapers and looking for other signs of dehydration and she didn’t show any, but we also knew it was a big threat as we were noting such little intake – a bowl of apple sauce and some ice chips here, a few sips of a water bottle there….it was scary. Believe me, I made her plates of every soft and appetizing food I could think of trying to get her to take a bite (and typically this girl can eat! you know something’s wrong when she is continually refusing food!) It was so sad to see her so miserable, she’d wake up whimpering and meltdown when Tyler left the room (she’s a major daddy’s girl). I had called the on call ENT after the night she threw up her medicine and he said to keep her on medicine and fluids (duh, but how!?) sometimes she’d get a partial dose in a few bites of applesauce or shaved ice. I did a ton of research online and confirmed that tonsillectomy’s are miserable and that the pain is terrible and sometimes days 5-7 are the worst…so I struggled wondering if this all was just part of the recovery (exacerbated by her not taking the meds). I read about the possibility of doing acetaminophen by suppository and we were relieved to try it – a piece of cake compared to taking oral meds at this point. The problem was that the dosage available over the counter was not a full dose for her weight, and it only lasts so long. Eventually, it was almost two days of barely taking anything and we called the ENT again and they said to take her to the ER. I dreaded the ER – mostly because I was afraid of long germ-filled waits, and having them not be able to do anything for her unless they put in an IV – she is the hardest girl to get a vein for blood draws or IVs (hence all the poke wounds from her surgery), it’s a miserable experience and traumatic for her every time. I wanted to avoid it at all costs! But with no better option and with being scared about not knowing what to do with her I hoped for the best when Tyler took her off to the hospital.
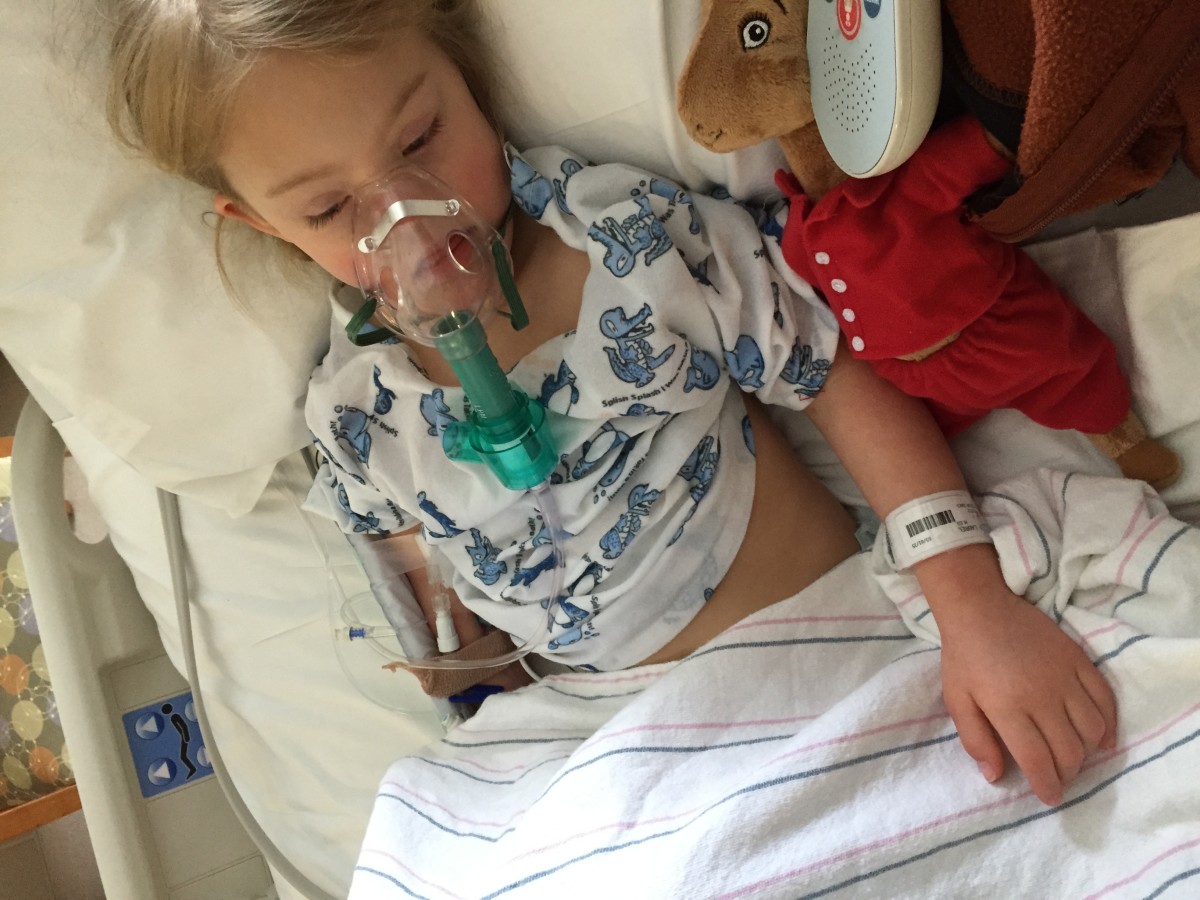
Our first family ER experience could not have gone more smoothly. He said he walked right in and was greeted by a triage nurse, the doctor came in shortly and they discovered she had pneumonia (!) and rather quickly they had a bed for her and got her started on an IV (the amazing nurse got it in on her first try – – even with her being so dehydrated!) and they had her on oxygen and were able to hook her up to monitor everything else to make sure she was okay. They determined she needed to be watched closely (it had gotten so bad!) and she was sent to the PICU. This was Sunday night. Tyler stayed with her basically around the clock while I managed Dylan and tried to get myself into decent shape (my allergies were terrible and I had a cold with a bad cough – I’m guessing we all shared Dylan’s souvenir hospital germs – and we had over a week of really bad sleep waking up to give meds or to console a miserable child). It was scary how bad it got so fast. Whitney was on oxygen for a few days – not being able to breathe sufficiently on her own. She still wouldn’t eat or drink or take oral meds for a few days. Finally, she was moved to a normal hospital bed on Tuesday, was able to come off the oxygen and breathe on her own on Wednesday, and on Thursday she was able to eat a little and drink a little and walked enough on her weak wobbly Bambi legs to show she was able to come home. We hadn’t heard her speak or seen her smile in almost a week. And I can’t tell you how relieving and sweet it was to all be sleeping under the same roof last night. Pnuemonia is a bear and will take a while to clear, but already we are seeing so much of our little girl coming back. And I think her throat is starting to cooperate with her a little more (although I think that will also take a while to get back to normal). We are wiped out, but grateful to seemingly be on the other side of this mess. And we are so hopeful that as she recovers, Whitney will be hearing, sleeping, and in general just breathing and feeling far better than she has in a long while.
Moral of the story: wait to schedule surgery until you can leave your restless young germ-magnet kid at home lest he lick the hospital hallway wall (no joke, this did happen, to my horror – don’t judge, I’d like to have seen you try to anticipate it and stop him in time). Also, don’t get off the round the clock pain meds after a tonsillectomy until you’re sure your kid is ready. And if your baby is miserable just take them in (this may seem obvious, but I have a strong tendency toward the wait it out, it’s probably about to get better, don’t risk wasting time money and energy if it can be avoided).
A few extra photos I wanted to add —
a low point…Whitney miserable, resting on our bed. I had brought an assortment of every soft food I hoped to be appetizing and she refused to touch anything.
Tonsillectomy food: smoothie, soft scrambled eggs (I added a little milk), mashed potatoes, oatmeal, apple sauce, yogurt
This is a photo the day she came home from the [2nd trip to the] hospital: she’s back to playing with her dolls and play kitchen. I know when her throat is hurting her, though, because she’ll do this with her mouth. It will be closed with a little bit of tongue showing and she’s doing everything she can not to swallow. She’ll play and sometimes crack a smile (keeping the pursed lips) but then if she coughs or tries to talk whatever has been pooling up in there comes out. Cute, but not so cute. 










Wow, what a wild roller coaster ride you were all on!!!
I m so glad to hear that everyone made it through safe and sound.
Hope Whitney is hearing, sleeping and just all around feeling better now.
xxxxxooooo
Yep, it has been one for the books for sure. I’m so glad the worst is over! She’s still recovering, but is so much more herself. Thanks for all your love and prayers!
M&T: I’m so sorry to hear it was such a difficult time with getting poor Whitney feeling better. We were praying for you all, but didn’t know how bad it was. I have to say you guys continue to impress me with how well you parent!
Sheesh! What an ordeal! You must be wiped out. Gosh, I wish I could’ve helped somehow… You and Tyler are AMAZING parents.
Your writing always makes me cry and smile. Thank you for sharing your journey with all of us. So thankful for Whitney’s recovery!